Treating Psoriasis: A Comprehensive Guide
- posted: Jun. 12, 2025
Treating Psoriasis: A Comprehensive Guide
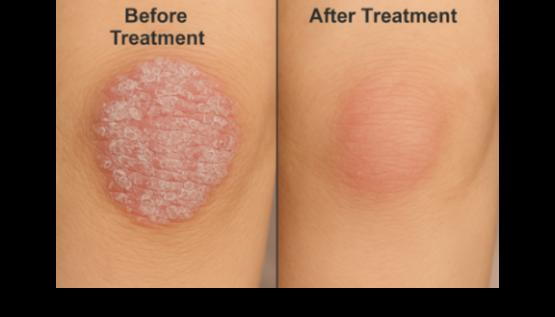
Psoriasis is a chronic, immune-mediated inflammatory skin condition that causes skin cells to multiply too quickly. This leads to thick, red, scaly patches that can appear anywhere on the body, most commonly on the scalp, elbows, knees, and lower back. Psoriasis tends to come and go, with periods of flare-ups followed by times of remission. While it isn't contagious, it can significantly affect a person's comfort, confidence, and quality of life.
There are several types of psoriasis, the most common being plaque psoriasis. Others include guttate, inverse, pustular, and erythrodermic psoriasis, each requiring slightly different treatment approaches. Triggers can include stress, infections, skin injuries, certain medications, and environmental factors.
Treatment Options
Psoriasis treatment varies depending on how severe the condition is and each person’s unique needs. Options range from over-the-counter products to prescription medications and light therapy. Most patients need a combination of approaches to manage flares and maintain long-term control.
Over-the-Counter Support
For milder symptoms, over-the-counter products can help soothe the skin and reduce scaling:
- Coal tar: Found in shampoos, creams, and bath soaks, coal tar helps slow skin cell growth and ease itching and inflammation.
- Salicylic acid: Helps soften and remove thick scale, allowing other treatments to work better.
- Moisturizers: Daily use of emollients with ceramides, urea, or lactic acid can reduce dryness, scaling, and irritation.
Topical Prescription Treatments
Topical therapies are often the first choice for mild to moderate psoriasis:
- Corticosteroids: These reduce inflammation and itching. Stronger formulas are used for thicker plaques, while lower-strength versions are used in sensitive areas like the face or groin.
- Vitamin D analogs: Such as calcipotriene or calcitriol, these help slow down overactive skin cell growth and are often combined with topical steroids.
- Calcineurin inhibitors: Like tacrolimus or pimecrolimus, these are used off-label in delicate areas where steroids might be too harsh.
- PDE-4 inhibitors: Roflumilast cream/ foam is a newer option that helps reduce inflammation, especially in folds of the skin.
Systemic Treatments (Oral or Injectable)
When psoriasis is more widespread or doesn’t respond to topical therapy, systemic medications may be used.
Oral options include:
- Apremilast (Otezla): A non-immunosuppressive pill that reduces inflammation through a unique pathway.
- Deucravacitinib (Soytyktu): A TYK2 inhibitor that targets a key enzyme in the immune response and offers an alternative to biologic injections.
- Methotrexate, cyclosporine, or acitretin: These older treatments are still used in certain cases but require regular monitoring due to potential side effects.
Biologics (injections or infusions) have transformed psoriasis care by targeting specific parts of the immune system. These include:
- TNF-alpha inhibitors: Like adalimumab (Humira) or etanercept (Enbrel)
- IL-17 inhibitors: Like secukinumab (Cosentyx) or ixekizumab (Taltz)
- IL-23 inhibitors: Such as guselkumab (Tremfya) and Risankizumab (
- IL-12/23 inhibitor: Ustekinumab (Stelara)
Biologics are often used for moderate to severe psoriasis and psoriatic arthritis, and many patients achieve clear or nearly clear skin.
Phototherapy
Light therapy can be a highly effective option, especially for patients who prefer to avoid systemic medications. Narrowband UVB is the most commonly used form and helps slow skin cell turnover. In-office sessions are typically done several times per week. For small, stubborn areas like the scalp or hands, an excimer laser may be used for more targeted treatment.
Lifestyle Support
Daily habits and overall health can make a big difference in managing psoriasis.
- Moisturize regularly to reduce flaking and discomfort
- Reduce stress, which can trigger flares
- Avoid smoking and limit alcohol, as both may worsen symptoms
- Maintain a healthy weight and consider an anti-inflammatory diet rich in whole foods and omega-3s
Individualized Care
Psoriasis treatment is highly individualized. What works for one person may not work for another, and treatments may need to be adjusted over time. Regular follow-ups with a dermatologist are essential to monitor progress, manage side effects, and tailor the approach as needed.
Conclusion
While there is no cure for psoriasis, it is a manageable condition. Advances in medical therapy have made it possible for many patients to achieve clear or nearly clear skin. With the right combination of treatments and lifestyle adjustments, individuals with psoriasis can lead comfortable, confident lives.

